The stroke continuum model below describes the elements of stroke care that patients and families experience on their journey with stroke. Your journey recovering after stroke will be unique and may not be a straight line through this continuum.
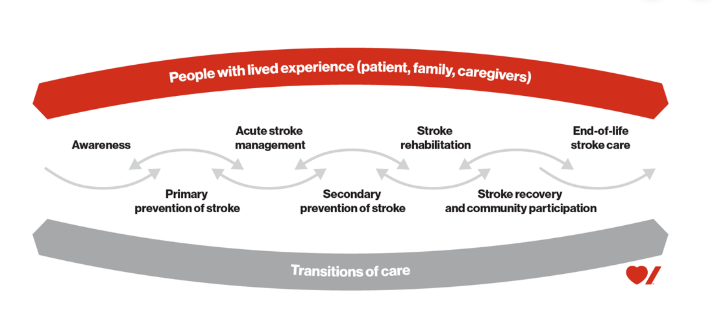
Awareness is about giving people the information they need to recognize and respond to stroke.
Primary prevention of stroke means managing risk factors to stop a first stroke or TIA event from happening. It usually happens in the home or in community based settings such as your family doctor’s office, when a doctor, nurse, pharmacist or patient starts a conversation about reducing stroke risk.
Acute stroke management generally refers to the care you receive within the first five to seven days after a stroke. This includes the hyper-acute and acute phases of stroke care.
Hyper-acute care focuses on urgent assessment to identify the type and cause of the stroke. Where possible, it focuses on reducing the impact of the stroke and protecting the brain with medical therapies.
Acute care focuses on medical management of the stroke, initial assessment by the multidisciplinary team, and planning for the next phase of care to promote recovery.
Secondary prevention of stroke is managing known risk factors to prevent another stroke or TIA from happening. Secondary prevention can take place in a variety of settings, including acute care, stroke prevention clinics, and community-based care settings such as your family doctor’s office.
Stroke rehabilitation is the active, assisted, and goal-directed recovery process that generally occurs over the first few months after stroke. Stroke rehabilitation helps people continue to live as independently as possible after a stroke, and to adjust to the physical and mental changes caused by a stroke. In stroke rehab, a team of health professionals works with a patient to regain skills lost as the result of a stroke. Rehab starts in the hospital and continues at a rehab centre or at home.
Stroke recovery and community participation is when a person is no longer actively involved with the health care system and is resuming their day-to-day life after stroke.
End-of-life stroke care is the management and care for patients and families when stroke results in death. This may occur early after the stroke or may be some time later as a result of complications from the stroke.
Transitions in care happen between each of these stages. The periods of transition can be unsettling times as people adapt to living with stroke. Talking with your doctor and health care team to ensure that you and your family are prepared for upcoming transitions can help them feel more successful.
The
Heart and Stroke Foundation and
Stroke Recovery Association of BC have a number of guides, videos and listings of community resources and services to help you navigate your way through the continuum of stroke care.

